Cervical & Lumbar Spondylosis Treatment in Nagpur
Advanced care for neck and back spine degeneration, offering relief from pain, stiffness, and nerve compression with modern treatments.
What is Cervical and Lumbar Spondylosis?
Cervical and lumbar spondylosis are age-related degenerative conditions affecting the spine. Cervical spondylosis impacts the neck vertebrae, while lumbar spondylosis affects the lower back. Over time, discs lose flexibility, vertebrae experience wear and tear, and spinal ligaments thicken, which may lead to stiffness, chronic pain, and nerve compression.
Early diagnosis and management help prevent worsening symptoms and maintain spine function. These conditions are commonly seen in individuals over the age of 40, but can develop earlier due to lifestyle factors or injury.
Causes of Cervical & Lumbar Spondylosis
Cervical and lumbar spondylosis result from progressive wear and tear of the spinal components. These conditions often arise due to lifestyle, genetics, or physical strain over time.
Understanding the causes can help with early prevention and better management.
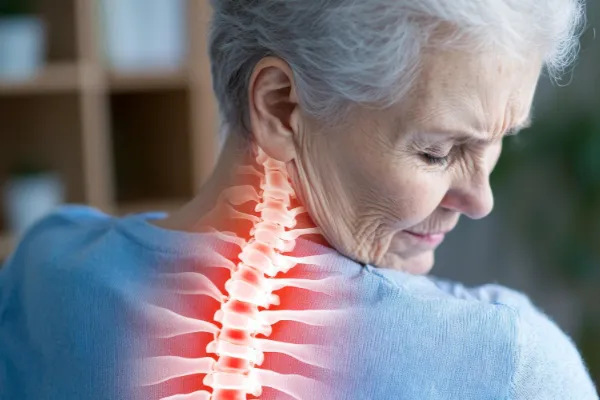
Age-Related Wear and Tear

Genetic Predisposition
Family history can increase the likelihood of developing spinal degeneration.

Poor Posture and Ergonomics

Obesity
Extra body weight accelerates spinal degeneration and increases pressure on discs.

Trauma or Injury
Past spinal injuries can trigger or accelerate spondylosis.

Repetitive Stress
Jobs or activities involving bending, lifting, or twisting increase the risk.
Symptoms of Cervical & Lumbar Spondylosis
Symptoms of spondylosis arise as spinal structures deteriorate and nerves become compressed. They can range from mild discomfort to debilitating pain and mobility issues. Early recognition of these signs can support timely intervention and relief.
Symptoms vary depending on the location and severity of degeneration. Common signs include:

Neck or Back Stiffness
Difficulty turning the neck or bending the back, often worse in the morning.

Chronic Pain

Numbness or Tingling

Weakness in Limbs
Muscle weakness due to nerve pressure, affecting grip or walking.
Headaches
Cervical spondylosis can sometimes cause tension headaches or dizziness.

Reduced Flexibility
Limited spine movement impacting daily activities.
Diagnosis of Spondylosis
Diagnosing spondylosis involves identifying the extent and location of spinal degeneration. A combination of clinical evaluation and imaging helps pinpoint the root cause of symptoms. Timely diagnosis is key to preventing complications and guiding treatment.
Accurate diagnosis is essential for effective treatment:
Medical history and symptom assessment:
Physical examination:
Imaging tests:
X-rays, MRI, or CT scans reveal disc degeneration, bone spurs, and nerve compression.
Neurological evaluation:
Treatment for Cervical & Lumbar Spondylosis
Treatment focuses on relieving pain, restoring mobility, and preventing further degeneration. Options range from lifestyle changes and therapy to medications or surgery in severe cases. A tailored approach ensures better symptom control and long-term spine health.
Non-Surgical Treatments
Non-surgical approaches are usually the first line of treatment to manage symptoms conservatively. They aim to reduce pain, restore function, and delay or avoid the need for surgery.
Medications:
Pain relievers, anti-inflammatory drugs, and muscle relaxants manage discomfort and swelling. These help control flare-ups and support daily function.
Physiotherapy:
Exercises improve posture, strengthen muscles, and restore flexibility to reduce nerve pressure. Regular sessions can prevent further spine deterioration.
Lifestyle modifications:
Maintaining a healthy weight, ergonomic adjustments, and activity modifications support recovery. Long-term habits play a crucial role in symptom control.
Epidural steroid injections:
Percutaneous Discectomy:
A minimally invasive technique in which a small portion of the damaged disc is removed using specialized instruments inserted through a tiny incision. It is suitable for selected cases and is typically performed on an outpatient basis with minimal downtime.
Surgical Treatments
Decompression surgery:
Removes bone spurs or disc material pressing on nerves. This helps to relieve nerve irritation and improve mobility.
Spinal fusion:
Artificial disc replacement:
Maintains spine mobility while replacing damaged discs. This preserves natural spine movement compared to fusion.
Minimally invasive procedures:
Keyhole approaches reduce tissue damage, pain, and recovery time. Patients typically experience shorter hospital stays and faster rehabilitation.
Recovery & Rehabilitation
Recovery varies based on how advanced the spondylosis is and the treatment method used. A structured rehabilitation plan helps restore strength, flexibility, and function after treatment. Proper recovery support can significantly improve long-term outcomes and quality of life.
Recovery depends on the severity and type of treatment:
- Rest and gradual activity: Light movement prevents stiffness without stressing the spine.
- Physiotherapy sessions: Focused exercises restore flexibility, strength, and posture.
- Pain management: Medications and targeted therapies help control discomfort during healing.
- Lifestyle guidance: Proper posture, spine-friendly habits, and weight management support long-term spine health.
- Post-surgery care: Wound monitoring, follow-up visits, and activity restrictions ensure safe recovery.
Relieve Your Spine Pain and Improve Mobility Today
If neck or back pain, stiffness, or nerve issues are affecting your life, don’t wait. Get expert evaluation and advanced treatment for cervical and lumbar spondylosis in Nagpur to restore comfort and mobility.
Frequently Asked Questions
Yes, without proper management, cervical or lumbar spondylosis can lead to increased stiffness, chronic pain, and nerve compression, potentially causing weakness or reduced mobility.
Absolutely. Physiotherapy, posture correction, medications, and lifestyle modifications often relieve pain, improve flexibility, and slow disease progression.
Symptom relief varies. Some patients notice improvement within days to weeks with conservative care, while post-surgical recovery may take several weeks to months for full benefits.
Yes. Nerve compression from degenerative changes can lead to tingling, numbness, or weakness in the limbs, requiring prompt evaluation to prevent permanent nerve damage.
Yes. Post-surgical physiotherapy strengthens supporting muscles, improves posture, and helps restore full spinal function, which is crucial for long-term recovery.
With proper treatment and lifestyle changes, most patients maintain mobility and continue regular activities. Severe cases may require activity adjustments to prevent flare-ups.
Maintaining good posture, regular exercise, a healthy weight, and ergonomic work practices help reduce spinal stress and slow degeneration.
Yes, chronic pain and stiffness can disrupt sleep and daily activities. Timely treatment, pain management, and physiotherapy improve comfort and overall quality of life.
